A Guide to Your Digestive System
Before we walk through your gut test results, it helps to review the major organs in your digestive system. At Clarity Health, we believe that knowledge is power and having a basic understanding of how your gut works can help you make sense of your symptoms. Below is a map of the whole system, so you can orient yourself before we look at your results together.
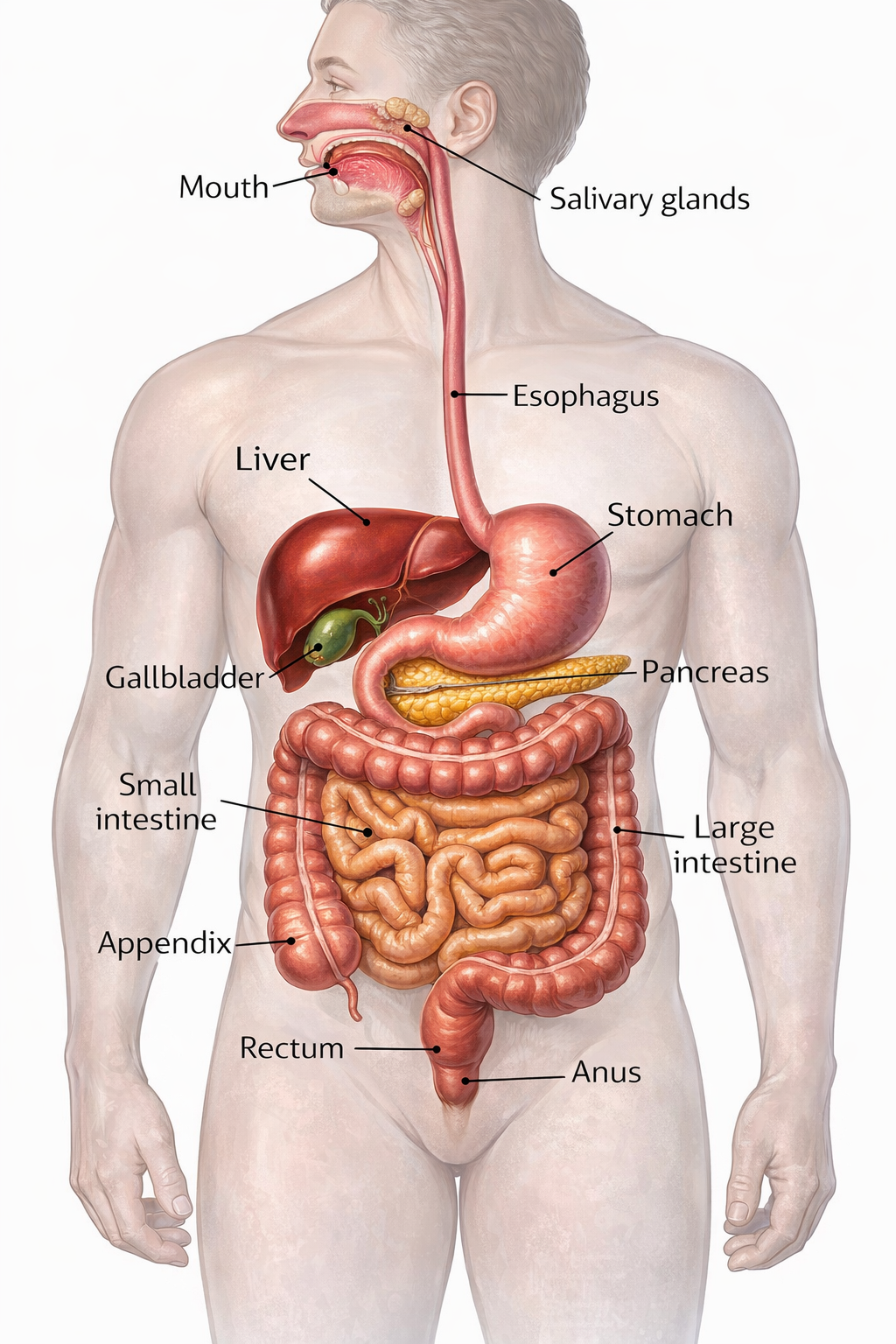
Section 1: The Digestive System at a Glance
Digestion is a coordinated process that relies on muscles, nerves, enzymes, and digestive secretions working together. Each step of the digestive tract influences each other, it requires a lot of things to go right for things to work as they should. This also means there are a lot of places where things can go wrong!
The primary digestive tract includes the mouth, esophagus, stomach, small intestine, large intestine (colon), and rectum. Supporting this process are three essential organs that do not directly carry food, but play a central role in digestion: the liver, gallbladder, and pancreas.
A key principle to keep in mind is that dysfunction earlier in the digestive process often shows up later. When digestion is impaired upstream, the downstream effects may be delayed, and sometimes appear in unexpected ways.
Section 2: The Digestive Tract, Step by Step
Mouth
Digestion begins in the mouth, where chewing mechanically breaks food down and saliva begins carbohydrate digestion. From there, the esophagus moves food into the stomach through coordinated muscular contractions. Even though this stage can feel basic, it sets the foundation for everything that follows. When chewing is incomplete, later stages of digestion have to compensate, and symptoms such as bloating and indigestion are more likely.
Stomach
The stomach performs two major functions: it breaks down protein using stomach acid and prepares food for the small intestine. It also acts as an important barrier against microbes that enter through food. In addition, the stomach signals downstream organs, especially the gallbladder and pancreas, to release digestive secretions. While many people assume reflux or upper abdominal discomfort always reflects excessive stomach acid, low stomach acid can also contribute to symptoms because food is not broken down efficiently or emptied in a timely manner. Common signs of impaired stomach function can include early bloating after meals, a heavy “food sits there” sensation, or reflux.
Small Intestine
The small intestine is where the majority of nutrient absorption occurs. Here, food is mixed with bile from the gallbladder and digestive enzymes from the pancreas, allowing fats, proteins, and carbohydrates to be broken down into absorbable components.
The small intestine also relies on coordinated muscular movements, known as peristalsis, to move contents forward. This process is supported by the migrating motor complex, a self-cleaning wave that sweeps the small intestine between meals. When this movement is disrupted, bacteria may accumulate where they do not belong, often referred to as bacterial overgrowth. This contributes to bloating, abdominal discomfort, irregular stool patterns, and in some cases fatigue or brain fog. When absorption is compromised, many people notice the impact outside of digestion, in energy, mood, and mental clarity.
Large Intestine
The large intestine (colon) absorbs water, forms and stores stool, and houses most of the gut microbiome. Microbes in the colon help ferment fiber and produce compounds that influence immune and nervous system signaling. The speed of transit through the colon strongly affects symptoms: slower transit allows more water reabsorption and tends to contribute to constipation, while faster transit reduces water reabsorption and can lead to loose stools or diarrhea. Because the colon interacts closely with immune and nervous system pathways, imbalance here can sometimes correlate with broader symptoms such as skin issues, immune changes, or mood shifts.
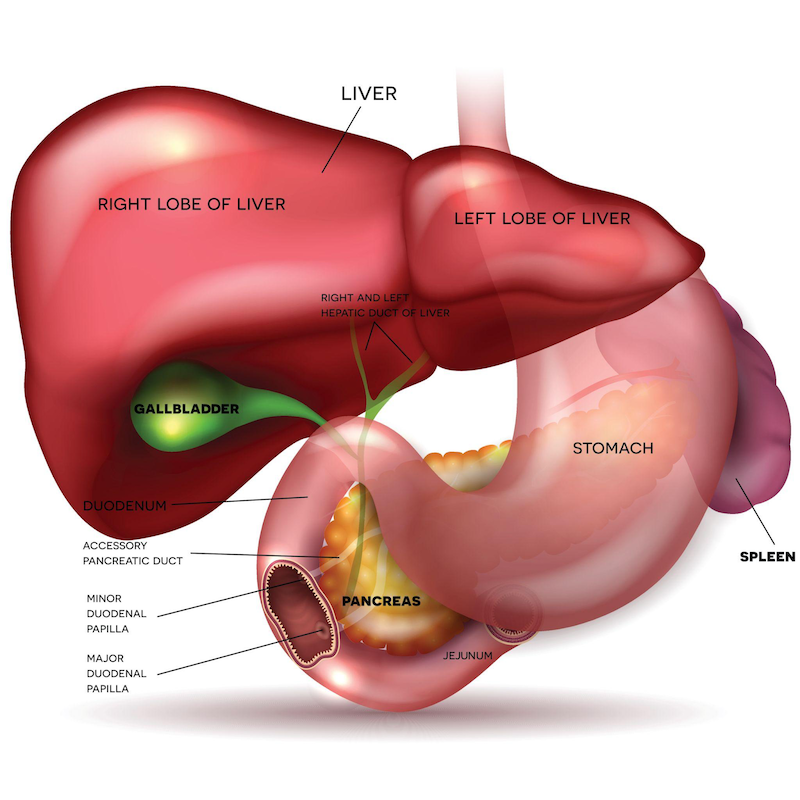
Section 3: Liver, gallbladder and pancreas
The liver, gallbladder, and pancreas rarely receive attention unless something is clearly “wrong,” yet they have an outsized impact on how digestion feels day to day.
Liver
The liver serves as a major processing and metabolic hub. In the context of digestion, it produces bile and helps process metabolic byproducts, medications, and hormones. When your body absorbs nutrients through the gut, the liver is the first stop. This is why, if your gut is having challenges like inflammation or bacterial overgrowth it can put an added demand on the liver.
The liver also plays key roles beyond digestion, including blood sugar regulation, production of critical proteins, such as albumin and clotting factors. The liver plays a primary role in cholesterol and hormone balance. In many ways, the liver functions like a processing center that supports multiple body systems simultaneously.
Gallbladder
The gallbladder stores and concentrates bile made by the liver and releases it in response to meals, especially meals containing fat. Bile is essential for fat digestion and absorption, including absorption of fat-soluble vitamins. It also supports healthy intestinal transit and plays an important role in bowel regularity. In addition, bile is one of the primary vehicles for eliminating metabolic waste filtered by the liver, and it helps regulate microbial balance in the gut. When bile flow is sluggish or insufficient, it may contribute to constipation, impaired fat digestion, nausea, dysbiosis, and, over time, gallstone formation. Gallbladder function is often overlooked unless gallstones are present, but bile flow can meaningfully influence everyday digestion.
Pancreas
The pancreas releases digestive enzymes that break down proteins, carbohydrates, and fats—performing much of the enzymatic work required to convert food into absorbable nutrients. The pancreas also plays a separate but related role in blood sugar regulation. When enzyme output is insufficient, people may experience gas, bloating, a sense of heaviness after meals, or signs of incomplete digestion such as visible undigested food in stool. Efficient digestion depends on coordinated function across the liver, gallbladder, and pancreas.
Conclusion: How This Guides Your Care
At Clarity Health, we believe education is a foundational ingredient in building long-term health resilience. When your gut test flags something, it's not just a number, it's a signal from a specific part of this system, and knowing which part helps you understand what to do about it.The better you understand how your digestive system works, the more clearly you can interpret what your body is communicating.
At Clarity, we use your symptoms as meaningful clinical inputs to help identify which parts of your digestive system may be impaired. By evaluating patterns in bloating, bowel habits, reflux, fatigue, or brain fog, alongside advanced testing, your clinician works with you to determine what those signals suggest about function in the stomach, small intestine, colon, liver, gallbladder, or pancreas.
Through your partnership with Clarity Health, you’ll begin to see how each test, recommendation, and adjustment connects back to restoring proper digestive function. Your clinician is there to guide you at every step — helping you interpret the data, understand the patterns, and move forward with clarity and confidence.
We look forward to seeing you at your next visit!




.svg)






